Postpartum memories are like glitter - they stick to everything and resurface when you least expect them.
Here’s my confession: I have two sons, now 13 and 11 - and yes, I’m more than a decade late writing this; but I hope what I learned from my breastfeeding journey can help you now.
Breastfeeding: Lessons I Learned the Hard Way (so you don’t have to)

When I had my boys, the postpartum world looked very different. There were fewer perineal ice packs, hardly any conversation about maternal mental health and a lot more of that old chestnut: “Just sleep when the baby sleeps” (ha!).
Today, our feeds are full of doulas, nipple shield hacks, placenta smoothies and pumping tutorials. And while that’s progress - new mums need support - the endless scroll can feel overwhelming. Not all advice is helpful, and much of it contradicts itself. What I really needed - especially when it came to breastfeeding - wasn’t another gadget or hashtag. I needed someone to sit beside me, guide me, and show me how.
When birth throws you a curveball
For my first, I’d dreamt of a water birth in the home-from-home unit at St Thomas’s. Instead, I had an induction, an epidural, an episiotomy, a ventouse delivery (imagine a Dyson on your baby’s head), and a third-degree tear.
I was shell-shocked.
After all that, I thought the hardest part was over.
I was wrong.
No one told me I could review my birth notes with a midwife - something that would have helped me process what happened - or ask for a lactation consultant while still in hospital. That alone could have made a world of difference.
"Milk usually comes in around day three," explains Indira Lopez-Bassols, International Board Certified Lactation Consultant (IBCLC). "But interventions - and I’d had plenty - can push that back and disrupt how feeding gets started."
The good news? "Birth doesn’t always go to plan," she continues, "but with the right support, breastfeeding can be nature’s second chance. It can even be deeply healing."
"For some mothers - especially those with birth trauma or mental health struggles - breastfeeding can help them reconnect with their bodies and feel just how resourceful they really are," adds Emma Webster, NCT qualified Breastfeeding Counsellor, Doula, and Hypnobirthing Instructor.
Breastfeeding isn’t instinctive - it’s learned

I thought breastfeeding would be simple: pop baby on, bond, nourish, float into bliss.
Oh, how wrong I was.
"It takes four to six weeks to truly establish breastfeeding" says Indira
"Newborns feed little and often, not in neat three-hour windows," adds Alex Bollen, NCT Practitioner and Author of Motherdom: Breaking Free From Bad Science and Good Mother Myths. "Forget the cleaning, get comfortable, put Netflix on if you feel like it and give yourself permission to simply be with your baby. "Without a tribe to clean, cook, and hold the fort this might seem impossible. The trick is to have a postnatal plan - to rope in as much help as possible from friends, family or professionals so you can focus on feeding and bonding.
In those early weeks, my son seemed to latch for hours on end but never looked full. I felt exhausted and inadequate. Much later, I learned he wasn’t really feeding the whole time - just nibbling - and that comfort sucking is normal. It’s also how your baby signals to your body what to produce. A trained breastfeeding counsellor or consultant would have spotted this straight away, reassured me, and helped me adjust his latch if needed.
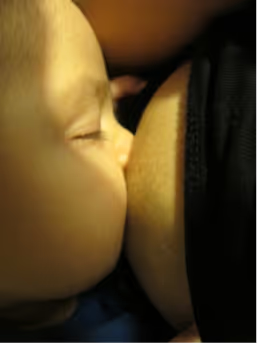
Looking back, I wish I’d given myself more grace - and more time. Through tears, I rushed to supplement with formula at week three, thinking I’d failed. What I really needed was space to learn and a helping hand.
"Learning to breastfeed is like learning to dance the tango," says Indira. "Two steps forward, one step back. But with the right support, you can absolutely do it."
"You’re learning, and so is your baby - it’s all about repetition," says Emma. "That’s why skin-to-skin is so important. Once you’re out of theatre and in a calm space, keep your baby on your skin for as long as you can. It helps them through the nine stages of getting familiar with feeding and releases hormones, like oxytocin and prolactin, that support milk production."
Her top tip? "Stay skin-to-skin as long as you feel comfortable - and if midwives or staff ask to take the baby for checks, it’s perfectly OK to say you need more time. You do have a voice."
We know that milk production is about demand and supply, and it takes practice. Indira stresses the importance of offering both breasts at each feed - a common mistake is offering just one. "The more you offer the more you produce.”
Pumps and tribulations
I tried pumping too - not because anyone advised me to, but because it seemed like all anyone talked about.
Desperate to kickstart my milk supply, I’d hunch over, willing my body to produce something - anything. Two sad ounces (which is normal by the way!) and three hours later, I’d cry. No one told me that if your baby feeds eight times a day, you need to pump and feed just as often to maintain supply. After one exhausting session, the idea of doing more felt impossible.
Looking back, I wish I’d sought proper advice instead of reaching straight for the pump. Social media constantly pushes all kinds of gadgets at us, but the truth is, not everyone needs them - and if you do, it’s worth getting guidance on what’s right for you at that stage.
“In today’s on-demand world, you can have anything delivered in 24 hours, so I always advise parents not to buy a pump before the baby arrives,” says Emma. “Wait until you actually need one - and choose what’s right for you at that point, because your needs can change throughout your breastfeeding journey.”
When grit isn’t enough
By the time my second son arrived - via planned C-section after my first birth left my pelvic floor in tatters. I was determined to succeed. But grit only takes you so far.
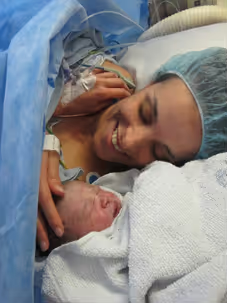
Again, I couldn’t manage exclusive breastfeeding. He lost a significant amount of weight in the first week, and I panicked. I began combination feeding with formula.
What I didn’t know then: if you’ve struggled before, you’re likely to struggle again - and you’re entitled to NHS breastfeeding support from day one.
I also didn’t know milk often comes in late after a C-section, and that learning to hand-express antenatally can help.
"Don’t wait until day two when your baby’s crying and you’re sore to learn," advises Indira.
Some women even harvest colostrum during late pregnancy to bridge the gap - though always check with your healthcare team first.
The good news: You are not a failure
I blamed my body for not being able to exclusively breastfeed.
But it wasn’t my body - it was the lack of support.
"Most people stop breastfeeding not because they can’t," says Indira, "but because they don’t get the right support. The system is failing them."
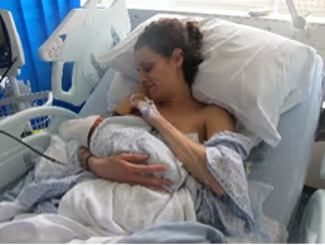
Pain, sore nipples, poor latch and low milk supply (perceived or actual) are common breastfeeding challenges, and often lead women to stop. But with the right guidance, many of these issues can be addressed early on.
“Women may find it impossible to trust their bodies, particularly if their birth was challenging,” adds Emma. "Some rely on apps to know when to feed and get overwhelmed by conflicting advice. My advice? Trust yourself. Keep a simple log of feeds and nappies for the first two weeks. If your baby has plenty of wet and dirty nappies, you’re doing just fine - better than any app can tell you."
And if breastfeeding simply isn’t possible? That’s okay too. There are many reasons: breast surgery, IGT (insufficient glandular tissue), trauma, medication, eating disorders, or simply not wanting to.
"We hold up the self-sacrificing mother as the gold standard," says Alex. "But that can be damaging. For some mums, breastfeeding difficulties can contribute to depression - they feel like a failure, and they can spiral downwards. I’d say it’s far better to be a well Mum bottle-feeding than a depressed mum struggling to breastfeed."
Food writer Yasmin Khan put it beautifully in her Vogue essay: after miscarriages, a traumatic birth, an IGT diagnosis, and several unsuccessful attempts to breastfeed, she chose weaning - not breastfeeding - as her healing process.
Her words helped me reframe motherhood - because it’s different for everyone.
Finding your village
Here’s the truth: good breastfeeding support exists - but it’s not always easy to find.
Every NHS hospital has an infant feeding team, but breastfeeding qualifications are not required, so the level of support varies depending on the Trust. Some NHS staff are trained in lactation, some aren’t. Some hospitals even have International Board Certified Lactation Consultants (IBCLCs) - the gold standard- but many don’t. So always ask.
Breastfeeding Counsellors (BFCs) - who also have formal training - are worth their weight in gold and often volunteer at drop-ins and baby cafés or can be hired privately.
Peer support is also invaluable. Drop-ins, helplines, baby cafés - great for practical tips, reassurance, encouragement, and perspective.
"Our role is to hold space for mothers," says Emma. "We give them the time to ‘dance the dance’ with their baby - guiding them, answering questions, and connecting them with others who’ve been there."
"Many first-time mums have never even seen breastfeeding in real life," says Alex. "Drop-ins show you what’s normal. We’re told it should be a beautiful bonding experience - but it can also feel stressful, even upsetting. None of that means you’re failing. It’s all normal."
For more complex situations - like low or oversupply, persistent pain, tongue tie or jaundice - it’s worth seeing an IBCLC. You can either ask to be referred on the NHS or hire one privately.
"We don’t just fix latches," says Indira. "We look at your full clinical history, birth, baby, mental health - and create a plan that works for you."
Final thoughts: If I could rewind time
Well, I wouldn’t - because I’ve made my peace with my breastfeeding journey. I made the best decisions I could with the information I had, and combi-feeding turned out to be right for me at the time. I still got to breastfeed and treasure those quiet hours with just me and my babies.
But if I knew then what I know now, I would have reached out for help much sooner - leaned on my healthcare team, popped into drop-ins, spoken to a Breastfeeding Counsellor, and asked for an IBCLC referral, especially knowing I had a planned C-section coming up.
Not because I was failing - but because I deserved support.
And so do you.
Breastfeeding might be natural - but that doesn’t mean it’s easy.
You’re not doing it wrong. You’re just doing something hard.
If you want to breastfeed, don’t give up straight away. Get help. It can make all the difference.
Whether you breastfeed, bottle-feed, pump, or mix it up - you deserve support.
Your journey is your own.
And it is enough.

Indira Lopez-Bassols - International Board Certified Lactation Consultant: indirayoga.com and Breastfeeding London

Emma Webster - NCT qualified Breastfeeding Counsellor, Doula and Hypnobirthing Instructor: surreyborn.com

Alex Bollen - NCT Practitioner and Author of Motherdom: Breaking Free From Bad Science and Good Mother Myths: motherdom.net